Aminoglycosides: Difference between revisions
From IDWiki
(→�) |
No edit summary |
||
| (8 intermediate revisions by the same user not shown) | |||
| Line 1: | Line 1: | ||
| − | == |
+ | ==Background== |
| + | *Derived from [[Streptomyces]] (mycins & kacins) or [[Micromonospora]] (micins) |
||
| − | === Initial === |
||
| + | ===Mechanism of Action=== |
||
| − | If actual body weight more than 20% higher than ideal body weight, need to calculate adjusted body weight (ABW) |
||
| + | *Requires electron transport chain (ETC) to cross over the membrane |
||
| − | $$ABW = IBW + 0.4 \times (actual BW - IBW)$$ |
||
| + | **Anaerobes are therefore inherently resistant |
||
| + | *Reversibly binds 30S ribosomal subunit, which stops proofreading and causes accumulation of bad proteins |
||
| + | ===Spectrum of Activity=== |
||
| − | === Traditional q8h dosing === |
||
| + | *Good coverage of Gram-negative aerobes |
||
| − | * Used for Enterococcus IE, meningitis, septic shock, ascites, AKI/CKD, prefnancy, surgical prophylaxis, burns, osteomyelitis |
||
| + | **Except [[Stenotrophomonas]] and [[Burkholderia]] |
||
| − | * 1.7mg/kg (5-7.5mg/kg amikacin) |
||
| + | *[[Streptomycin]] also covers mycobacterium |
||
| + | *Some protozoal coverage |
||
| + | *Can cover Gram-positives if cell wall is disrupted (e.g. by beta-lactam) |
||
| + | ===Mechanisms of Resistance=== |
||
| − | === Extended interval dosing === |
||
| + | *Altered 50S ribosomal subunit |
||
| − | * 7mg/kg (15mg/kg amikacin) |
||
| + | *Decreased uptake and accumulation ([[Pseudomonas]]) |
||
| − | * Use Hartford nomogram with a random level (but remember to halve the amikacin level first) |
||
| + | *Decreased membrane permeability |
||
| − | * CrCl ≥60 q24h |
||
| + | *Efflux pump ([[Escherichia coli]]) |
||
| − | * CrCl 40-59 q36h |
||
| + | *Aminoglycoside-modifying enzymes ([[Enterococcus]]) |
||
| − | * CrCl 20-39 q48h |
||
| − | * CrCl ≤19 don't use |
||
| + | ===Pharmacokinetics and Pharmacodynamics=== |
||
| − | === Dialysis === |
||
| + | *Poor membrane penetration, therefore doesn't cross over into lungs and CSF |
||
| − | * Pre-HD levels with post-HD doses, though this may change |
||
| + | *Half-life 2-3 hours (longer in CKD) |
||
| + | *Excreted 99% unchanged in urine |
||
| + | *Displays concentration-depedent killing with a prolonged post-antibiotic effect (2-13 hours) |
||
| − | == |
+ | ==Dosing== |
| + | ===Initial Dose=== |
||
| − | * 1mg/kg divided q8-12h, peak target 3-5, trough <2 |
||
| + | *If actual body weight more than 20% higher than [https://www.mdcalc.com/ideal-body-weight-adjusted-body-weight ideal body weight], need to calculate [https://www.mdcalc.com/ideal-body-weight-adjusted-body-weight adjusted body weight] (ABW) |
||
| − | === Monitoring === |
||
| + | $$ABW = IBW + 0.4 \times (actual BW - IBW)$$ |
||
| − | === Peak === |
||
| + | ===Traditional Dosing=== |
||
| − | * 30min after third? dose |
||
| − | * Response is based on peak:MIC ratio, target is 8-10 times |
||
| − | * If below target, increase dose |
||
| + | *Q8H dosing |
||
| − | === Trough === |
||
| + | *Used for [[Enterococcus]] IE, [[meningitis]], [[septic shock]], [[ascites]], [[AKI]]/[[CKD]], [[pregnancy]], surgical prophylaxis, [[Burn infection|burns]], [[osteomyelitis]] |
||
| + | *1.7 mg/kg (5-7.5 mg/kg [[amikacin]]) IV q8h |
||
| + | ===Extended Interval Dosing=== |
||
| − | * Prior to 4th dose, or a random level at 24-48h in renal failure |
||
| − | * Side effects are predicted by trough levels |
||
| − | * Tobra <0.5 (extended) or <2 (traditional) |
||
| − | * Amikacin <1 (extended) or <?? (traditional) |
||
| − | * If above target, increase interval |
||
| + | *Q24H dosing, which is safer but less well-studied |
||
| − | === Hartford Nomogram === |
||
| + | *7 mg/kg (15 mg/kg [[amikacin]]) IV, frequency depends on [[CrCl]] |
||
| + | **[[CrCl]] ≥60 q24h |
||
| + | **[https://www.mdcalc.com/creatinine-clearance-cockcroft-gault-equation CrCl] 40-59 q36h |
||
| + | **[https://www.mdcalc.com/creatinine-clearance-cockcroft-gault-equation CrCl] 20-39 q48h |
||
| + | **[https://www.mdcalc.com/creatinine-clearance-cockcroft-gault-equation CrCl] ≤19 don't use |
||
| + | *Use [[Hartford nomogram]] with a random level (but remember to halve the [[amikacin]] level first) |
||
| + | ===Dialysis Dosing=== |
||
| − | [[File:Hartford_nomogram.png]] |
||
| + | *Pre-HD levels with post-HD doses, though this may change |
||
| − | Double the concentration for [[amikacin]] |
||
| − | == |
+ | ===Synergy=== |
| + | *1 mg/kg divided q8-12h, peak target 3-5, trough <2 |
||
| − | * Derived from [[Streptomyces species]] (mycins & kacins) or [[Micromonospora species]] (micins) |
||
| − | == |
+ | ===Monitoring=== |
| + | ====Peak==== |
||
| − | * Requires electron transport chain (ETC) to cross over the membrane |
||
| − | ** Anaerobes are therefore inherently resistant |
||
| − | * Reversibly binds 30S ribosomal subunit, which stops proofreading and causes accumulation of bad proteins |
||
| + | *30 minutes after third dose |
||
| − | == Spectrum of Activity == |
||
| + | *Response is based on peak:MIC ratio, target is 8-10 times |
||
| + | *If below target, increase dose |
||
| + | ====Trough==== |
||
| − | * Good coverage of Gram-negative aerobes |
||
| − | ** Except Stenotrophomonas and Burkholderia |
||
| − | * Streptomycin also covers mycobacterium |
||
| − | * Some protozoal coverage |
||
| − | * Can cover Gram-positives if cell wall is disrupted (e.g. by beta-lactam) |
||
| + | *Prior to 4th dose, or a random level at 24 to 48h in renal failure |
||
| − | == Resistance == |
||
| + | *Side effects are predicted by trough levels |
||
| + | *[[Tobramycin]] <0.5 (extended) or <2 (traditional) |
||
| + | *[[Amikacin]] <1 (extended) or <?? (traditional) |
||
| + | *If above target, increase interval |
||
| + | ====Hartford Nomogram==== |
||
| − | * Altered 50S ribosomal subunit |
||
| + | |||
| − | * Decreased uptake and accumulation (Pseudomonas) |
||
| + | [[File:Hartford_nomogram.png]] |
||
| − | * Decreased membrane permeability |
||
| − | * Efflux (E. coli) |
||
| − | * Aminoglycoside-modifying enzymes (Enterococcus) |
||
| + | *Dosing interval is whichever is the line just above the random level |
||
| − | == PK/PD == |
||
| + | *Double the concentration for [[amikacin]] |
||
| + | ==Safety== |
||
| − | * Poor membrane penetration, therefore doesn't cross over into lungs and CSF |
||
| − | * Half-life 2-3 hours (longer in CKD) |
||
| − | * Excreted 99% unchanged in urine |
||
| − | * Displays concentration-depedent killing with a prolonged post-antibiotic effect (2-13 hours) |
||
| + | ===Adverse Drug Reactions=== |
||
| − | == Side Effects == |
||
| − | * |
+ | *Nephrotoxicity (0-50%), usually non-oliguric AKI with decreased Ca/Mg resorption, often reversible |
| − | ** |
+ | **Decreased protein synthesis |
| − | ** |
+ | **Decreased cellular respiration |
| − | ** |
+ | **Increased apoptosis |
| − | ** |
+ | **Necrosis in proximal tubules |
| − | * |
+ | *Ototoxicity (0-60%), irreversible |
| − | ** |
+ | **Cumulative effect |
| − | ** |
+ | **Distribute into the perilymph of the ear, and cause free radical formation causing apoptosis of hair cells |
| − | ** |
+ | **Needs hearing tests, because it can be subclinical |
| − | *** |
+ | ***Monitor audiometry weekly |
| − | * |
+ | *Vestibulotoxicity (0-20%), irreversible |
| − | * |
+ | *Rarely, neuromuscular blockade |
| − | == |
+ | ===Monitoring=== |
| − | * |
+ | *Trough levels |
| − | * |
+ | *Creatinine |
| − | * |
+ | *Weekly audiometry |
[[Category:Antibiotics]] |
[[Category:Antibiotics]] |
||
Latest revision as of 14:46, 11 January 2024
Background
- Derived from Streptomyces (mycins & kacins) or Micromonospora (micins)
Mechanism of Action
- Requires electron transport chain (ETC) to cross over the membrane
- Anaerobes are therefore inherently resistant
- Reversibly binds 30S ribosomal subunit, which stops proofreading and causes accumulation of bad proteins
Spectrum of Activity
- Good coverage of Gram-negative aerobes
- Except Stenotrophomonas and Burkholderia
- Streptomycin also covers mycobacterium
- Some protozoal coverage
- Can cover Gram-positives if cell wall is disrupted (e.g. by beta-lactam)
Mechanisms of Resistance
- Altered 50S ribosomal subunit
- Decreased uptake and accumulation (Pseudomonas)
- Decreased membrane permeability
- Efflux pump (Escherichia coli)
- Aminoglycoside-modifying enzymes (Enterococcus)
Pharmacokinetics and Pharmacodynamics
- Poor membrane penetration, therefore doesn't cross over into lungs and CSF
- Half-life 2-3 hours (longer in CKD)
- Excreted 99% unchanged in urine
- Displays concentration-depedent killing with a prolonged post-antibiotic effect (2-13 hours)
Dosing
Initial Dose
- If actual body weight more than 20% higher than ideal body weight, need to calculate adjusted body weight (ABW)
$$ABW = IBW + 0.4 \times (actual BW - IBW)$$
Traditional Dosing
- Q8H dosing
- Used for Enterococcus IE, meningitis, septic shock, ascites, AKI/CKD, pregnancy, surgical prophylaxis, burns, osteomyelitis
- 1.7 mg/kg (5-7.5 mg/kg amikacin) IV q8h
Extended Interval Dosing
- Q24H dosing, which is safer but less well-studied
- 7 mg/kg (15 mg/kg amikacin) IV, frequency depends on CrCl
- Use Hartford nomogram with a random level (but remember to halve the amikacin level first)
Dialysis Dosing
- Pre-HD levels with post-HD doses, though this may change
Synergy
- 1 mg/kg divided q8-12h, peak target 3-5, trough <2
Monitoring
Peak
- 30 minutes after third dose
- Response is based on peak:MIC ratio, target is 8-10 times
- If below target, increase dose
Trough
- Prior to 4th dose, or a random level at 24 to 48h in renal failure
- Side effects are predicted by trough levels
- Tobramycin <0.5 (extended) or <2 (traditional)
- Amikacin <1 (extended) or <?? (traditional)
- If above target, increase interval
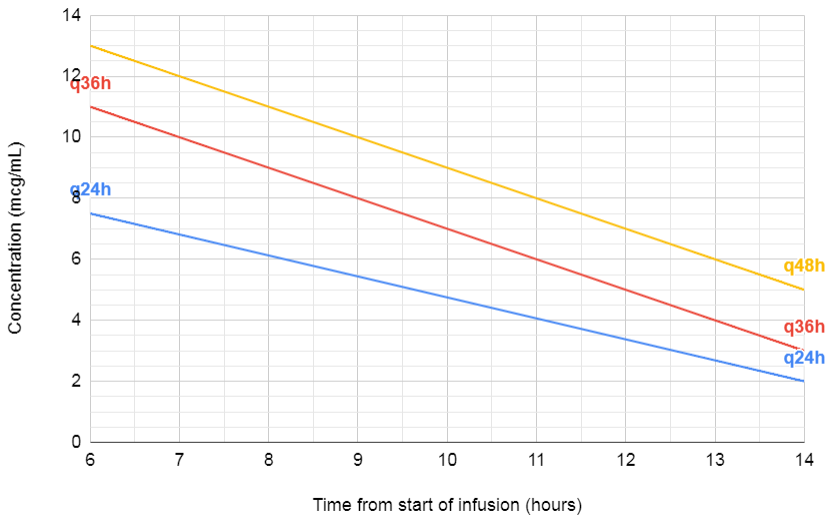
Hartford Nomogram
- Dosing interval is whichever is the line just above the random level
- Double the concentration for amikacin
Safety
Adverse Drug Reactions
- Nephrotoxicity (0-50%), usually non-oliguric AKI with decreased Ca/Mg resorption, often reversible
- Decreased protein synthesis
- Decreased cellular respiration
- Increased apoptosis
- Necrosis in proximal tubules
- Ototoxicity (0-60%), irreversible
- Cumulative effect
- Distribute into the perilymph of the ear, and cause free radical formation causing apoptosis of hair cells
- Needs hearing tests, because it can be subclinical
- Monitor audiometry weekly
- Vestibulotoxicity (0-20%), irreversible
- Rarely, neuromuscular blockade
Monitoring
- Trough levels
- Creatinine
- Weekly audiometry